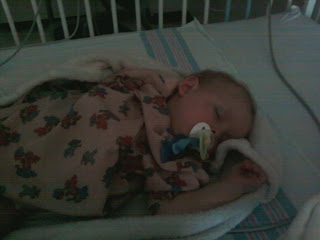
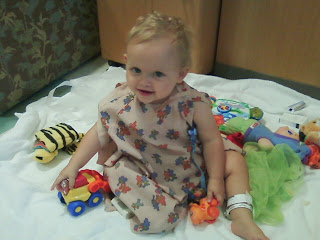
Currently Chase is doing well although he has some unresolved issues. He is still passing blood in his stool, but not as much as he was before the probiotics. He has high blood pressure that has been documented since he was about 6 months old. His blood work still shows anemia, metabolic acidosis, low CO2 and high platelets. He passes undigested food daily and his skin is always powdery and salty. He has developed PICA, believed to be a result of his inability to absorb nutrients. He eats chalk, dirt, sand, soap, paper, leaves and anything else he can get his hands on. He drinks water constantly and he has hyperpigmentation in his skin.
On a recent visit to the beach, Chase drunk the salt water constantly. We couln't make him stop.
His chronic cough has gotten better and he is no longer stooling 20 times a day. He does still have diarrhea, but the high doses of iron he takes helps. He receives therapy twice a week, physical therapy and occupational therapy. He is hypotonic, so PT works on his mobility. They have helped so much and he began sitting at 9 months and walking at 14 months. They are also signing with him as he is a bit delayed in his communication skills. His occupational therapist helps with his inability to eat and swallow normally. At 14 months, he began to eat a few mashed foods. He gags on everything and at 16 months is still only able to eat a few things. Some days he may eat 2 bites of food and some days as much as 10 or 15 bites of food. His main source of nutrition is still breastmilk. He nursed every 2 hours around the clock until he was 12 months old. Since then and as he has started to eat more, he goes about 4 hours during the day and 3 hours at night between feedings.
A few weeks ago, Chase got a new GI doctor at the hospital we are established at. She seemed very intrigued with his issues and told us she would be consulting with other doctors before our next visit with her. He also seen a new nephrologist. They are reluctant to put him on blood pressure medicine since it is dehydrating and sedating in some cases. At our next visit with them they are going to do an ultrasound of his kidneys because of the metabolic acidosis and an echo cardiogram to make sure the blood pressure is not enlarging his heart.
I have tremendous faith that God will see Chase through all of this and he will outgrow it all. In the meantime, I feel it is my job alone to ensure he is followed as closely as needed and nothing is missed. Chase is such a happy little fellow. He smiles all the time and constantly reminds me of both the complexity and simplicity of life. God has blessed us as a family so much it is hard to put it into words. It is my goal everyday to live for my Jesus and praise him for all he has done.
Our Angel

Chase Maddox
Wednesday, September 28, 2011
On our own...again.
We left the GI follow-up visit so discouraged. I began digging for someone to help us and connected with a doctor out of state who seemed to know about PHA. I learned our insurance would not pay for the out of state care, so that was not an option for us. At this time, our GI doctor had released us telling us again Chase just had allergies. The genetic tests had not come back yet. We did not have a nephrologist and our PCP was less than helpful. We did however have a hematologist who was involved in Chase's care because of his bloodwork abnormalities. We went to see her and took the pictures of Chase's ulcers along with our worries. She was adamant that we get a second opinion for his GI issues and even helped us get referred in a collaborative care program at the hospital. A second opinion meant traveling to another children's hospital in our state. We tried to get the appointments set up through the standard referral service, but the closest appointment we could get was 6 weeks out. The next day, Chase began to scream in pain every time his bowels moved and the blood was increasing. I took him to his PCP and again they were no help. I just continued to pray that God would help me make the right decisions as his mother. At wits end, I called the PCP's office back and asked them to try to get us an appointment sooner that the 6 weeks they initially told us. They were unable to and told me just to take him to the ER. So, at 4 am the following day we packed our bags and made the 3 hour trip. It was one of the best decisions we have ever made. Even though we felt like we were on our own about all of this, God was there. He had a perfect plan, we just had to have faith.
We were admitted and for the next 5 days Chase had a great team of doctors digging into his medical history and his current condition. Having read a case study of an infant with PHA dying of and unexplained bowel perforation, we were mainly there for them to rule out it was about to happen with Chase. They were not sure why he had the ulcers, but they were able to help us rule out that Chase suffered from food allergies. The nephrologist there also made a theoretical connection between the amount of salt he was wasting to his bowels and the ulcers lining his colon. They were interestingly intrigued at the rarity of PHA and seemed to want to learn something from Chase, which is just what we had been looking for someone to do. God is so good!!! We were released having ruled out several GI disorders and allergies. They put Chase on an adult dose of probiotics which have seemed to help tremendously.
We were admitted and for the next 5 days Chase had a great team of doctors digging into his medical history and his current condition. Having read a case study of an infant with PHA dying of and unexplained bowel perforation, we were mainly there for them to rule out it was about to happen with Chase. They were not sure why he had the ulcers, but they were able to help us rule out that Chase suffered from food allergies. The nephrologist there also made a theoretical connection between the amount of salt he was wasting to his bowels and the ulcers lining his colon. They were interestingly intrigued at the rarity of PHA and seemed to want to learn something from Chase, which is just what we had been looking for someone to do. God is so good!!! We were released having ruled out several GI disorders and allergies. They put Chase on an adult dose of probiotics which have seemed to help tremendously.
Monday, September 26, 2011
A developmental evaluation did prove he was about 12 standard deviations behind for his age. His developmental doctor referred us to a geneticist for review of Chase's medical history and to follow up on the PHA diagnosis. At the same time we were referred to a hematologist because of his consistently abnormal bloodwork. His platelets were almost 1 million, he was anemic, had metabolic acidosis, an elevated WBC, and all of his kidney functions were outside the normal range. His sodium remained on the low end of normal and his potassium on the high end of normal. This is also the time his first high blood pressure was documented. A further look at his anemia with an iron profile showed he was completely depleted of stores in his blood. The hematologist put him on high doses of iron and has been following him closely since. The geneticist was very thorough and confirmed the PHA diagnosis based on clinical criteria. Blood samples were taken (this was a horrible process Chase had to endure) and genetic tests were conducted in Weisswasser, Germany. Since then, Chase has been hospitalized twice for a total of 9 days. He also underwent 2 cystic fibrosis sweat tests. Both of which he had a bad reaction to and sustained chemical burns. The administrator said she had been testing children for 27 years and had never seen anything like it. The test results came back normal.
The GI doctor decided to do a colonoscopy and found large ulcers lining his colon, which we think is the source of the blood. Preparing him for this was horrible. It was an inpatient preparation and the enemas he had to endure caused blood clots to pass from his colon and just fall out of him on the sheets in his crib. I think that was the most pain I have ever had to see him in. After the colonoscopy, the GI doctor who has been practicing for almost 30 years apologized to us for saying all this time Chase had enteropothy and allergies. He then told us he had never seen anything like the ulcers and promised to consult with other GI doctors and look into the effects of PHA on his colon before our follow-up visit. We had so much hope and thought finally, someone was going to put some of these puzzle pieces together for us. Well...he didn't. At the follow-up appointment, he began talking about allergies again.
Waiting to be admitted for dehydration at 10 months. Like I said before...he smiles through it all :)
The GI doctor decided to do a colonoscopy and found large ulcers lining his colon, which we think is the source of the blood. Preparing him for this was horrible. It was an inpatient preparation and the enemas he had to endure caused blood clots to pass from his colon and just fall out of him on the sheets in his crib. I think that was the most pain I have ever had to see him in. After the colonoscopy, the GI doctor who has been practicing for almost 30 years apologized to us for saying all this time Chase had enteropothy and allergies. He then told us he had never seen anything like the ulcers and promised to consult with other GI doctors and look into the effects of PHA on his colon before our follow-up visit. We had so much hope and thought finally, someone was going to put some of these puzzle pieces together for us. Well...he didn't. At the follow-up appointment, he began talking about allergies again.
Waiting to be admitted for dehydration at 10 months. Like I said before...he smiles through it all :)
Doing our best
For the next couple of months we kept Chase away from crowds as much as we could and I kept him hydrated the best I could. The bloody stools he had had in the hospital were black water. Now he was stooling bright red blood and continued to have profuse diarrhea. He continued to nurse every 1.5 to 2 hours around the clock and the number of stools were the same, around 20 per day. I talked to the PCP several times about the blood and we were being followed by a pediatric GI doctor. Chase's routine blood work was never within the normal range and he continued to sleep all the time. The GI doctor told us Chase was still dealing with post gastro enteropothy from the GI virus he was diagnosed with. Without a nephrologist and a GI doctor who was unwilling to research PHA, we were just giving it all to God. I placed ALL of my trust in God and I knew he was going to take care of Chase.
Shortly after he turned 6 months old we attempted to feed him baby food carrots. It was horrible. He screamed in pain and the stools were laced with more blood than I had seen before. We took pictures of the bloody diapers because it seemed that no one was listening to us. By this time he was actually stooling blood clots. We made a trip back to the GI doctor who said that Chase was now dealing with a word I have grown to shiver at when I hear it...allergies. So just to sum it all up...we almost lost our baby to a GI virus that lasted for two weeks at its initial onset. Then, he was suffering from post gastro enteropothy for 5 months because of this GI virus he had and now he has developed allergies...oh my the frustration level at this point was beyond bad. Why would no one help us? And why would no one take a closer look...because he was gaining weight. Actually, the reason he was gaining weight was because I was with him all day keeping a log of his ins and outs and up with him all night nursing him every 2 hours around the clock. I was also up changing his diaper all night just trying to keep the diarrhea off of him. His little bottom was so raw and blistered from the diarrhea and he was so weak he could barely stay awake. At 7 months old, Chase had just learned to roll over and was far from sitting up. He vocalized very little and we could tell his development was not like Aubrianna's had been. But he did smile...he smiled all the time. He was the happiest little baby I have ever seen. When he would smile, it would light up the room and I could just see the sweet spirit he had about him.
Shortly after he turned 6 months old we attempted to feed him baby food carrots. It was horrible. He screamed in pain and the stools were laced with more blood than I had seen before. We took pictures of the bloody diapers because it seemed that no one was listening to us. By this time he was actually stooling blood clots. We made a trip back to the GI doctor who said that Chase was now dealing with a word I have grown to shiver at when I hear it...allergies. So just to sum it all up...we almost lost our baby to a GI virus that lasted for two weeks at its initial onset. Then, he was suffering from post gastro enteropothy for 5 months because of this GI virus he had and now he has developed allergies...oh my the frustration level at this point was beyond bad. Why would no one help us? And why would no one take a closer look...because he was gaining weight. Actually, the reason he was gaining weight was because I was with him all day keeping a log of his ins and outs and up with him all night nursing him every 2 hours around the clock. I was also up changing his diaper all night just trying to keep the diarrhea off of him. His little bottom was so raw and blistered from the diarrhea and he was so weak he could barely stay awake. At 7 months old, Chase had just learned to roll over and was far from sitting up. He vocalized very little and we could tell his development was not like Aubrianna's had been. But he did smile...he smiled all the time. He was the happiest little baby I have ever seen. When he would smile, it would light up the room and I could just see the sweet spirit he had about him.
PHA or not?
We came home on a Tuesday night and Chase was still eating well. The next day we went to the PCP for a weight check. He had finally gained an ounce, but more importantly this was the first day he wasn't losing weight. He was nursing every 1.5 to 2 hours around the clock and having about 20 stools per day. The cough continued and the mucus in his chest and nose made made it hard for him to breathe. He continued to sleep for about 20 out of 24 hours. On Thursday the PCP called me at home to talk about his condition. She wasn't happy that we had been discharged and had been sorting through all of his discharge paperwork. She asked me again if anyone had given me a diagnosis and I told her no. Then she asked "they never told you he had pseudohypoaldosteronism?" I said pseudo what? She then began to spell it to me...I remember digging for a pen and writing what seemed like every letter in the alphabet as she spelled it out loud. She told me we were going back to the hospital clinic the following week to meet with the nephrologist. I immediately started searching the internet about PHA and wow...this was it - this was what was wrong with Chase. Why hadn't anyone mentioned this to us? Why didn't we know sooner and why did we have to wait a whole week to talk to the nephrologist about it?
We went to the appointment an were suprised when he told us he wanted to follow Chase closely for the next few weeks but he did not believe Chase had PHA. A couple of days after that visit his PCP called me back and said she was sending us to another nephrologist about 3 hours from home at another children's hospital. When we got there we met a nephrologist who told us he knew the nephrologist that had been following Chase because he had studied under him in medical school. He said "if he said Chase doesn't have PHA, then he doesn't". We really didn't know what to think other than we had wasted 6 hours of driving time, a whole day at the hospital and put Chase through more blood work and ultrasounds. So we returned home with our little Angel and I done the best I could to keep him hydrated.
One of Chase's first smiles at about 9 weeks old.
We went to the appointment an were suprised when he told us he wanted to follow Chase closely for the next few weeks but he did not believe Chase had PHA. A couple of days after that visit his PCP called me back and said she was sending us to another nephrologist about 3 hours from home at another children's hospital. When we got there we met a nephrologist who told us he knew the nephrologist that had been following Chase because he had studied under him in medical school. He said "if he said Chase doesn't have PHA, then he doesn't". We really didn't know what to think other than we had wasted 6 hours of driving time, a whole day at the hospital and put Chase through more blood work and ultrasounds. So we returned home with our little Angel and I done the best I could to keep him hydrated.
We began the 1 hour drive back to the Children's Hospital. Chase could barely hold his eyes open and he seemed to be having trouble breathing. Our PCP was trying to arrange a direct readmission for us, but things were not working out, as she was dealing with the same doctor who had discharged us just hours before. As we sat in the lobby waiting on the readmission, we were in constant contact with our PCP. She was concerned that we were running out of time on getting the fluids reconnected and told us just to get up and take him to the emergency department. The next few days were absolutely horrible for Chase. He endured hundreds of painful sticks including arterial sticks and an EJ line. He was choking on the oral sodium and still having bloody diarrhea, coughing, runs of tachycardia and barely keeping his eyes open.
This was so sad and so frustrating as a mother because he had just had a perfectly good central line pulled before we were sent home. The doctor was so unconcerned with what he was having to go through. He was miserable and still not getting much better. After 3 days of misery, he woke up and decided he wanted to nurse. This was on Sunday morning at 7 am. This was the first time he initiated nursing in about 2 weeks. Two hours later he wanted to nurse again and this trend continued throughout the day. They told us he now had post gastro enteropathy, basically saying he was over the virus and still having the symptoms because his intestines were damaged. We were discharged again after 5 days, but I did feel better about leaving this time since he was at least eating.
This was so sad and so frustrating as a mother because he had just had a perfectly good central line pulled before we were sent home. The doctor was so unconcerned with what he was having to go through. He was miserable and still not getting much better. After 3 days of misery, he woke up and decided he wanted to nurse. This was on Sunday morning at 7 am. This was the first time he initiated nursing in about 2 weeks. Two hours later he wanted to nurse again and this trend continued throughout the day. They told us he now had post gastro enteropathy, basically saying he was over the virus and still having the symptoms because his intestines were damaged. We were discharged again after 5 days, but I did feel better about leaving this time since he was at least eating.
Sunday, September 25, 2011
A change in doctors
The central line was wonderful and all day Saturday he slept well. They altered his TPN every 8 hours to make sure he was getting what he needed. Sunday morning he woke up and looked at us for the first time in 8 days like he knew who we were. Early Monday morning a mass began to form around the base of the central line. It had already failed for blood draws overnight, but the fluids were still running. They stopped the fluids and had to xray the line. After about 8 hours they were finally able to reconnect the fluids. Chase wasn't getting any better and this time without fluids set him back again. We were questioning everyone about his condition and a diagnosis. We had had a change in doctors and it just seemed they were not doing anything to find out what was making him so sick. A GI virus remained the diagnosis despite the other symptoms he was having. By this time he had lost about 20 % of his body weight and was still too weak to even open his eyes. His bloodwork was improving as a direct result of the TPN, but he was lifeless. We talked to the doctors about CF since it had been mentioned to us. They told us since he passed his newborn screen CF would be ruled out. They moved us out of the PICCU and decided he could begin nursing again. He was so weak he could barely latch, but I tried my best to keep him awake. The new doctor we had was far from the one we had upon admission. She was not easy to talk to and every question we asked she had a quick response to. She was adamant that Chase had a virus and was unwilling to check into anything else. On Thursday, I was told we were going to be discharged. They unhooked his TPN, pulled his central line and sent us home. I did ask for one more set of labs before we left, but she said it was not needed. I was so excited at the thought of going home...I just wanted all of this to be over and I missed my little Aubrianna so much that words could not describe it. I tried to tell myself that everything was ok, but I knew Chase was still so sick. We got home at around 8 pm on Thursday. I honestly sat up all night watching his condition deteriorate. As soon as his PCP's office was open on Friday, I took him in. I will never forget the look on the doctor's face as she walked into the room. She sent us immediately back to the local hospital for blood draws and told me to go home and repack our bags while she waited on the stat results. It was scary...his sodium was back to 123 and his potassium at 6.8.
Waiting on the xray results to check the status of his line.
Waiting on the xray results to check the status of his line.
Thursday, September 22, 2011
Just as Chase was beginning to get rehydrated, his veins decided they had had enough. They made him NPO to allow his bowels to rest, but he still needed nutrition and fluids. Our only option was a Central Line. For several hours they talked about how and who on the placement of the line. Chase was so weak the anesthesiologist did not feel comfortable putting him under general anesthesia. The plan became to do it with a sedative, ketamine. It took them six hours to decide they were going to do it and all of this time Chase was losing the bit of hydration he had gotten. As the team arrived to place the line, my sweet Moma led us in prayer. We just prayed God would guide the hands of the doctor and that Chase would not feel the pain. We left and waited. It seemed like it took them hours to come and get us. They let us go back as soon as it was placed while they waited on the xray team to check the placement. It was perfect. God is so good! They quickly got his fluids attached and got his TPN going. Now he could get his fluids, TPN, oral sodium and constant blood draws all from the ports in the central line. He now has 4 scars on his tiny shoulder where they placed the stitches at the base of the central line. Everytime I look at them I am so thankful. They are a constant reminder to me of how blessed we are to have our little guy still with us.
Chase rested really well after the line was placed. It was a side effect of the sedative they gave him, but the rest was important for him.
Chase rested really well after the line was placed. It was a side effect of the sedative they gave him, but the rest was important for him.
The yellow scrubs.
As gastrointestinal virus was an ok explanation for all of this for the first 24 hours, but as day 5 was approaching with worsening symptoms I knew it was something far worse. In the PICCU, we were in a glass room with Chase and the doctors and nurses were constantly coming to his bedside. Before they entered the glass door, they had to suit up in yellow scrubs due to the contact isolation Chase was under. I completely understand their intent of not transferring germs, but I knew what Chase had was not contagious. No one in our family had been sick and I had been by his side every second and I hadn't caught this GI virus. I remember watching them suit up and wondering why they still thought he had a virus and why they were not telling us anything else that it could possibly be. Stool cultures, urine cultures and blood cultures were all coming back negative. I learned later that day that part of the confusion was the manner in which we were transferred. Chase's PCP had transferred him as a stable patient with a GI virus. He listed that Chase was admitted for dehydration and that he was being transferred with corrected dehydration. Basically saying he was only transferring us because we requested it and not because Chase needed further medical care. The rest of this day is quite a blur, by this time I had been up for going on 72 hours. Chase's cough worsened and the tremors continued. After 14 hours of no urine in his cath, we finally seen a drop. They were collecting the black water he was passing to do additional stool tests. His MRI showed a tiny lesion in his brain which was probably caused by the amounts of sodium he was receiving. He had a hard time keeping the oxygen level in his blood normal and all night long he had bouts of tachycardia. The next morning his nurse came in and forgot her yellow suit. She realized it just as she approached Chase's bedside, but said "oh well, he doesn't have anything contagious or we would all be sick by now as bad as he is". I decided to pick her brain a bit on what she thought was wrong and she told me Cystic Fibrosis. As soon as she left Ryan and I started searching the Internet about CF. It was the first thing we had heard besides a GI virus and we wanted to learn more about it.
Tuesday, September 20, 2011
Angels All Around
We followed the ambulance on the one hour drive to the nearest children's hospital. It was a surreal drive...Ryan and I didn't talk much as we stayed steadily behind them. I think I just kept reading the name of the hospital on the back of the ambulance over and over and I felt like I couldn't breathe. They took Chase to a room on the 8th floor and we were met by the Doctor and his student in the room. As they introduced themselves, I remember them asking me how Chase looks to me. I could tell they knew he didn't look well, but since this was the first time they had ever seen him, I am sure they were just wanting my opinion. After a complete medical history and some blood draws, they left the room and told us they would be back. About and hour later, the whirlwind began. The door opened and the room flooded with people. The student that had been with the doctor tried to talk to us and tell us what they were doing as more and more people kept coming in. At one point all I could do was count people (there were 22) because I couldn't even see Chase. We were trying to focus on answering all the new questions coming at us from the medical staff, but all I wanted to do was know what they were thinking. They told us his sodium was at 119 and potassium at 8.9, but we still didn't know what that meant. A team from the PICCU came from the 6th floor and he was quickly taken to their unit. The questions kept coming and when we got to the 6th floor. They were suiting up in yellow scrubs from head to toe and explained we would be under contact isolation as a precaution since the diarrhea was so bad. They explained to us the dangers of the potassium level and other tests they were about to perform. They quickly done and echo cardiogram to check for heart damage and to see how his heart was reacting to the potassium level. He was in hypovolemic shock and his heart was showing signs of tachycardia. The emergency response team came in and began trying for additional vein access for all the things they were about to run in his IV. For the next 3 hours Chase was stuck about 60 times as they tried time and time again for vein access. By this time it was about 4 AM and Ryan and I were just staring at our Baby. He had lost the ability to cry at this point and just gave up and went to sleep. There were so many different IV's they had to bring in another pole and pump to hook them all up.
At around 7 AM some of the Doctors came by to do initial consultations with Chase. The "tremors" he was having were thought to be seizures by now. His kidneys were shutting down and he had quit producing urine. They cathed him in hopes of measuring and sampling any urine he could produce. The diarrhea was non-stop and by now he was just passing black water (blood). They explained to us they were resuscitating him with the fluids and had to give him dangerous ammounts of sodium in a short ammount of time. They followed the sodium boluses with an MRI to check for brain lesions. Chase had metabolic acidosis, aldosterone level in the thousands (normal 5 to 30), elevated renin and a WBC at 35 thousand. All we could do was stand by his little crib and watch all the monitiors constantly beeping. The staff was trying to keep us informed about their plan, but no one knew what was wrong with him. We were at their mercy and just prayed God would guide them. When I look back on this day and even these pictures, I see my sick baby, but I also see Angels. Angels that rode with him as he was transported, held him all night as they worked with him, and guided the decisions of the doctors as they resuscitated him.
At around 7 AM some of the Doctors came by to do initial consultations with Chase. The "tremors" he was having were thought to be seizures by now. His kidneys were shutting down and he had quit producing urine. They cathed him in hopes of measuring and sampling any urine he could produce. The diarrhea was non-stop and by now he was just passing black water (blood). They explained to us they were resuscitating him with the fluids and had to give him dangerous ammounts of sodium in a short ammount of time. They followed the sodium boluses with an MRI to check for brain lesions. Chase had metabolic acidosis, aldosterone level in the thousands (normal 5 to 30), elevated renin and a WBC at 35 thousand. All we could do was stand by his little crib and watch all the monitiors constantly beeping. The staff was trying to keep us informed about their plan, but no one knew what was wrong with him. We were at their mercy and just prayed God would guide them. When I look back on this day and even these pictures, I see my sick baby, but I also see Angels. Angels that rode with him as he was transported, held him all night as they worked with him, and guided the decisions of the doctors as they resuscitated him.
Thursday, September 15, 2011
Our first learning curve in healthcare...
We were admitted to the local hospital with Chase on a Monday afternoon after spending all day in the ER with him. After 13 attempts they were finally able to get a 1 cc blood draw and start IV fluids. I stood back and prayed as they stuck him time after time that God would just take the pain away. I was scared, but relieved they were able to finally get the fluids going. I honestly thought we would get the fluids overnight and he would be doing better by the next day. On Tuesday, he continued to get worse and my suspicions of the medical staff's inability to care for Chase began to build. My thoughts initially were that Chase was sick, but at least we were in the hospital where he could get fluids and get over this GI virus. As the hours passed and he wasn't getting better, I began to worry more and question the nurses. His pediatrician had only visited him once and the nurses were not able to get any vitals on him because they didn't have any infant equipment and one even told me he "didn't do babies". I tried to keep calm and focused on keeping track on all of Chase's ins and outs...it was alarming to say the least, but we were still being told he had a GI virus and it just had to run it course. Tuesday night is very hard for me to think about now and some of the images of my lifeless baby will never leave my mind. He was getting so bad that he started turning a grayish color and even blue at times. His cough continued to get worse and the vomiting and diarrhea were non-stop. I sat with him all night dipping his passi in water and letting it drip in his parched mouth. The nurses were no help, so I just held him and counted down the hours before the doctor would be back the next morning. When the doctor arrived he said "so Chase is doing better?". I asked him what he meant and he said the nurses told him the symptoms had improved overnight. Furthermore, I had kept a very detailed list of his ins and outs and they told the doctor they lost it. With my baby beginning to have "tremors" all over his body, turning gray and absolutely unable to open his eyes I asked to be transferred to a Children's hospital about an hour away. Had I known it was going to take them 6 hours to get us there I would have ran out the door with Chase and taken him myself. In hindsight, I would have handled these three days so much differently. God has a perfect plan and we must always remember that. I have to or I would go crazy over the images these days have left me with.
Wednesday, September 14, 2011
The day it all began...
On July 3, 2010 we were at a family gathering to celebrate Independance Day. This picture was taken just hours before we would take Chase to the ER for the first time. I am going to try to start from the beginning as it all plays into the big picture. I knew from a few hours after Chase was born that he was different. Being my second born I had his sister to compare him to and when he had passed his 12th stool in the 15 hours since his birth, I knew something was wrong. He had trouble keeping his body temperature up and his blood sugar stayed low for the first couple of days. Since he was born premature, he had to pass a car seat test before we could bring him home. He failed this test miserably and I remember the nurse creeping back into the room with our baby to tell us about it. This meant he could not hold his oxygen level above 90% while in his car seat. So, we purchase a car bed that allowed him to lay flat for the car ride home. When we got home, we noticed he could not sit at all in a reclined position, like in a bouncy seat or swing. He would turn blue until he was laid flat again. The stooling continued to be excessive, up to 20 times per day, but the PCP continued to tell me it was normal since he was breastfeeding every 1 1/2 to 2 hours around the clock. Chase slept if he wasn't nursing and when he did latch he would go back to sleep. He also had lots of mucus in his nose and chest and was developing a productive and hacking cough. On this day in July he also started vomiting. With the stools being non-stop and the vomiting, I knew something was wrong and after a call to the nurse we headed to the ER. They done a quick exam and sent us back home. They told us to return if the vomiting continued. He got worse as the night went on and we returned the next morning. The doctor in the ER decided to admit us and said Chase had a GI virus. This was the beginning of the hospital stays...
Why we are sharing our story...
As the very blessed mother of a healthy 3 year old little girl, Aubrianna, I was overcome with excitement the day she was born. My life changed forever that day in July of 2008. Almost every mother I knew had given me their account of what motherhood was like. I listened to each and every one of them and smiled thinking I understood exactly what they were talking about. Boy was I wrong. I didn't have a clue what motherhood would bring me. In an instant, my life became more than it had ever been and I couldn't have been more thankful. A healthy baby girl who exceeded all of my expectations and brought me joy every second of the day. Soon after her birth, I reluctantly returned to my job as a business professional and was miserable. I wanted to be home with her so bad, but it just wouldn't work out financially. I was very fortunate to work for a wonderful boss who helped me get a part time schedule for several months. I worked hard, but my heart was at home with my little girl. She grew quickly exceeding all of her developmental milestones and was a tiny, but healthy little thing. She caught a couple of common viruses as a toddler, but was otherwise healthy as could be. Her only visits to her PCP were for her infant check-ups and vaccinations. I felt so bad for her when I took her in for those vaccinations and would worry about them for days before she had to go in. Then I would worry about the low grade fever she had after them - a common response and sign of a good immune system. She has always developed new skills quickly and always been a social butterfly. I would soon learn that worrying about those simple things with Aubrianna, which seemed so big, were nothing compared to what we were about to experience with Chase. When Aubrianna was 13 months old we learned we were expecting another baby. We were of course thrilled and so thankful to God. Everything was perfect until about 19 weeks along in the pregnancy. On January 25th, 2010 our lives changed as preterm labor began. For the next 15 weeks I spent most of my time in the bed at home or in the hospital praying that God would just give our little baby one more day in the womb. On May 23, 2010 little Chase Maddox was born at 36 weeks gestation. A healthy and beautiful 5 lb and 1 oz blessing from God himself. After 3 days in the newborn nursery, we brought him home. We were so happy to have that 4 month journey behind us and so thankful to be bringing our baby home. I couldn't wait to get home and be done with the hospital stays. Unfortunately, I now know all of those hospital stays and scary days were just God's way of preparing us to handle what was to come. Chase is now 15 months old and such a little trooper. He has been diagnosed with Pseudohypoaldosteronism Type 1 Dominant (PHA1). Such a long and intimidating phrase...a phrase that keeps me awake every night and fills some of the minutes in my busy days. A phrase that no one seems to know much about which is why we are sharing our journey. I hope to help others by sharing our little Chase's story.
Subscribe to:
Comments (Atom)